
(908) 381-8160Berkeley Heights
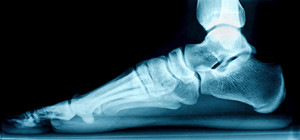
Flat feet, a common condition in adults, occurs when the arches of the feet collapse, causing the entire sole to touch the ground. This condition typically advances through several stages, each with its own set of symptoms. In the early stages, some individuals may not experience any discomfort or issues, while others may feel mild pain or fatigue after prolonged standing or physical activity. As flat feet progress, the discomfort can intensify, spreading to the ankles, knees, and lower back. This can result in reduced mobility and chronic pain. In severe cases, the arch completely flattens, and the foot loses flexibility, leading to a more pronounced disability. Recognizing the stages of flat feet is important for appropriate management, as early intervention can bring various choices of treatment to choose from. If you have flat feet, it is suggested that you are under the care of a podiatrist who can guide you toward appropriate relief methods.
Flatfoot is a condition many people suffer from. If you have flat feet, contact Dr. Janet Leicht from New Jersey. Our doctor will treat your foot and ankle needs.
What Are Flat Feet?
Flatfoot is a condition in which the arch of the foot is depressed and the sole of the foot is almost completely in contact with the ground. About 20-30% of the population generally has flat feet because their arches never formed during growth.
Conditions & Problems:
Having flat feet makes it difficult to run or walk because of the stress placed on the ankles.
Alignment – The general alignment of your legs can be disrupted, because the ankles move inward which can cause major discomfort.
Knees – If you have complications with your knees, flat feet can be a contributor to arthritis in that area.
Symptoms
Treatment
If you are experiencing pain and stress on the foot you may weaken the posterior tibial tendon, which runs around the inside of the ankle.
If you have any questions please feel free to contact our office located in Berkeley Heights, NJ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Flatfoot is a condition that occurs when the arches on the foot are flattened, which allows the soles of the feet to touch the floor. Flatfoot is a common condition and it is usually painless.
Throughout childhood, most people begin to develop arches in their feet, however, some do not. Those who do not develop arches are left with flatfoot. The pain associated with flat feet is usually at its worse when engaging in activity. Another symptom that may occur with those who have this condition is swelling along the inside of the ankle.
It is also possible to have flexible flatfoot. Flexible flatfoot occurs when the arch is visible while sitting or standing on the tiptoes, but it disappears when standing. People who have flexible flatfoot are often children and most outgrow it without any problems.
There are some risk factors that may make you more likely to develop flatfoot. Those who have diabetes and rheumatoid arthritis have an increased risk of flatfoot development. Other factors include aging and obesity.
Diagnosis for flat feet is usually done by a series of tests by your podiatrist. Your podiatrist will typically try an x-ray, CT scan, ultrasound, or MRI on the feet. Treatment is usually not necessary for flat foot unless it causes pain. However, therapy is often used for those who experience pain in their flat feet. Some other suggested treatment options are arch supports, stretching exercises, and supportive shoes.
Foot stress fractures, prevalent among runners, are primarily attributed to overuse, constituting 80 percent of cases. The repetitive forces during running may cause microscopic bone damage, escalating into hairline fractures if adequate recovery time is not provided. Sudden increases in running volume, intensity, or frequency, common in the overtraining syndrome, can make it worse. Running form also plays a role, especially with those who have a pronounced heel strike. However, transitioning abruptly to a forefoot strike or wearing minimal footwear can similarly increase the risk of metatarsal stress fractures. Nutrition is a vital factor in preventing stress fractures of the feet. Low vitamin D levels, specifically during winter, elevate the risk of stress fractures. Runners, especially women, face heightened risk if conditions such as osteoporosis or menstrual cycle-related amenorrhea are present. Additionally, sudden changes in running surfaces, such as switching from trails to roads without proper training, can elevate the risk. Wearing proper footwear is equally as important. Old, ill-fitting shoes that lack proper support can increase bone stress. Balancing training intensity, adopting gradual changes in running techniques, maintaining a nutritious diet, and ensuring proper footwear are key components of a comprehensive approach to foot health and injury prevention. For help in managing foot stress fractures, it is suggested that you schedule an appointment with a podiatrist.
Stress fractures occur when there is a tiny crack within a bone. To learn more, contact Dr. Janet Leicht from New Jersey. Our doctor can provide the care you need to keep you pain free and on your feet.
How Are They Caused?
Stress fractures are the result of repetitive force being placed on the bone. Since the lower leg and feet often carry most of the body’s weight, stress fractures are likely to occur in these areas. If you rush into a new exercise, you are more likely to develop a stress fracture since you are starting too much, too soon. Pain resulting from stress fractures may go unnoticed at first, however it may start to worsen over time.
Risk Factors
Stress fractures do not always heal properly, so it is important that you seek help from a podiatrist if you suspect you may have one. Ignoring your stress fracture may cause it to worsen, and you may develop chronic pain as well as additional fractures.
If you have any questions, please feel free to contact our office located in Berkeley Heights, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Our bones are important aspects of our body and they are constantly changing. The heavier the workload for a bone, the more likely it is that calcium will be placed in it. When a bone isn’t used often, there won’t be much calcium within it. When stress from repetitive loads prevent the bone from being able to repair itself, cracks will start to form. Stress fractures are defined as cracks in a bone that result from repetitive force, such as overuse.
The most common cause of stress fractures is a sudden increase in intensity and duration of physical activity. For example, if you begin to run long distances without working your way into doing so, you will be more likely to develop a stress fracture.
Common symptoms of stress fractures are pain and swelling near the weight bearing area on the injured bone. When initial x-rays are performed, it is possible that the fracture will not show up. However, once the stress on the area continues, the damage will increase, and the fracture will be severe enough to show up on an x-ray. Certain parts of the foot are more likely to develop stress fractures than others. Areas that typically have these fractures are: the metatarsals, the navicular bone, the calcaneus, tibia, and fibula.
Since women are at an increased risk of developing osteoporosis, they are twice as likely as men to sustain a stress fracture. Additionally, old age causes a decrease in bone mineral density which is why elderly people are also likely to develop these fractures.
It is important for you to be professionally diagnosed by a podiatrist if you suspect you have a stress fracture, because there are other injuries that can easily be mistaken for a fracture. Sprains, strains, shin splints, plantar fasciitis, and Morton’s neuroma can all easily be mistaken for stress fractures in the foot. Your podiatrist will likely ask you a series of questions to determine what type of pain you are experiencing. These questions will help your doctor identify whether you have a stress fracture.
The best method of treatment for a stress fracture is rest. Additionally, a walking boot, cast, or crutches, will help rest the area that is injured. The typical healing time for stress fractures is 4-12 weeks, however this depends on which bone is involved.
Limb salvage is a procedure that involves saving a lower extremity from amputation. In podiatry, limb amputation often occurs as a result of diabetes, peripheral vascular disease, neuropathy, cancer, and severe crush injury. The fundamental goal of limb salvage is to restore and maintain stability and movement of the affected lower extremity.
The procedure typically involves removing the diseased tissue and a small portion of the surrounding healthy tissue, as well as the removal of any affected bone if necessary. If the bone is removed, it is then replaced with prostheses, synthetic metal rods or plates, or grafts from either the patient’s body or a donor. Limb salvage is typically the preferred choice of procedure over amputation, as the procedure preserves both the patient’s appearance and allows for the greatest possible degree of function in the affected limb.
Upon diagnosis and determining that limb salvage is the appropriate treatment, the podiatrist may enlist the help of a physical and/or occupational therapist to prepare the patient for surgery by introducing various muscle-strengthening, walking, and range of motion exercises. Such exercises may be continued as rehabilitation post-procedure.

Approximately 60,000 lower extremity amputations are performed annually in the United States in patients with diabetes. This fact makes ulceration, infection, and gangrene a prevalent foot and ankle issue for diabetics people. Many amputations can be prevented through daily foot care habits and regular visits to a podiatrist to monitor foot ulcers. These experts suggest adopting an everyday foot care routine of inspecting the feet thoroughly for any changes in shape, color, sensation, or skin integrity. To prevent complications, podiatrists also recommend a gentle cleaning that involves washing feet in lukewarm water with mild soap, avoiding soaking, and ensuring thorough drying, especially between the toes. Nail care includes trimming nails straight across, avoiding rounding the corners. Callus management suggests gently reducing calluses with a foot file or pumice stone, rubbing in one direction to avoid skin tears. Diabetic patients should opt for cushioned, breathable shoes with soft uppers. Choosing cotton or natural fiber socks over synthetic materials is recommended. If you have diabetes, and are experiencing foot ulcers, it is suggested that you are under the care of a podiatrist who is medically trained to manage this condition.
Limb salvage can be an effective way in preventing the need for limb amputation. If you have diabetes, cancer, or any other condition that could lead to foot amputation if left unchecked, consult with Dr. Janet Leicht from New Jersey. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Limb Salvage?
Limb salvage is the attempt of saving a limb, such as the foot from amputation. Podiatrists also try to make sure that there is enough function in the foot after the salvage that it is still usable. Diabetes is the number one cause of non-traumatic amputations in the United States. Those with diabetes experience poor blood circulation, which prevents proper healing of an ulcer. If the ulcer is left uncheck, it could become infected, which could result in the need for amputation.
However, there are other causes as well, such as cancer and traumatic injury. Links between higher mortality rates and amputation have been found. This translates into higher healthcare costs, and a reduced quality of life and mobility for amputees. Podiatrists have attempted to increase the prevalence of limb salvage in an attempt to solve these issues.
Diagnosis and Treatment
Limb salvage teams have grown in recent years that utilize a number of different treatments to save the infected limb. This includes podiatrists that specialize in wound care, rehabilitation, orthotics, and surgery. Through a combination of these methods, limb salvage has been found to be an effective treatment for infected limbs, and as an alternative to amputation. Podiatrists will first evaluate the potential for limb salvage and determine if the limb can be saved or must be amputated.
If you have any questions, please feel free to contact our office located in Berkeley Heights, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Tendons are fibrous tissues that connect muscles with bone. The Achilles tendon is the largest tendon in the body. It connects the calf muscles at the back of the leg with the heel, and facilitates movements such as jumping, running, and walking.
Because the Achilles tendon is engaged so frequently and bears a great deal of pressure and stress throughout the day, it can become injured. Achilles tendon injuries cause the tissue to become irritated, inflamed, and swollen. Pain can come on gradually or be immediate, and will vary from mild to severe depending upon the injury. Where the pain occurs will vary as well, from just above the heel up through the back of the leg. There may also be stiffness in the tendon.
Achilles tendon injuries can often be caused by repetitive stress. They may also occur while running, playing tennis, gymnastics, football, basketball, dancing, soccer, baseball or other sports that require speeding up, slowing down, or pivoting quickly. Wearing high heels, falling from an elevation, stepping in a hole, having flat feet, bone spurs, tight leg muscles or tendons, wearing improper athletic shoes, exercising on uneven surfaces, or starting a new type of exercise can also cause Achilles tendon injuries.
The two most common Achilles tendon injuries are tendonitis and ruptures. Tendonitis causes painful inflammation and can occur in different parts of the tendon. Non-insertional Achilles tendonitis occurs when the fibers in middle of the tendon begin to break down, thicken, and swell. This condition typically affects younger, more active adults. Insertional Achilles tendonitis occurs where the tendon inserts into the heel bone. It is common for bone spurs to form with this type of injury. This condition can affect people of any age and level of activity.
Achilles tendon ruptures are a tear in the tendon. These breaks may be partial or complete. There may be an audible popping noise at the moment of injury and the pain will be sudden and severe.
An Achilles tendon injury can be diagnosed by your podiatrist after they examine you, check your range of motion, and possibly perform a calf squeeze test or review an X-ray or MRI. Depending on the type and severity of your injury, your podiatrist may treat your condition with rest/ice/compression/elevation (RICE), nonsteroidal anti-inflammatory medications, heel lifts, and stretching and strengthening exercises. If you have torn your Achilles tendon, treatment may include physical therapy, ultrasound, shockwave therapy, or possibly even surgery.
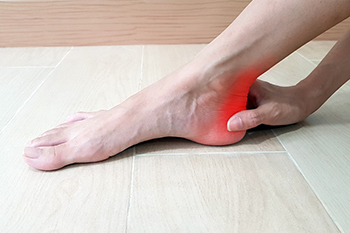
Achilles tendonitis is a common injury that affects both athletes and non-athletes alike. It is often the result of repeated stress on the Achilles tendon, the long tendon that connects the calf muscles to the heel. Achilles tendonitis primarily strikes the younger and middle-aged population engaged in sports like running, gymnastics, and basketball. But it can also affect those leading a more sedentary lifestyle. One of the leading causes stems from an abrupt surge in physical activity, leaving the body little time to acclimate to the increased strain. Failure to stretch adequately before engaging in activities such as running or jumping on hard surfaces can increase the risk, particularly for those with tight calf muscles. Footwear choices play a pivotal role in Achilles tendon health. Wearing high heels for extended periods without proper support can contribute to the onset of Achilles tendonitis. Factors like flat feet, obesity, diabetes, high blood pressure, and certain antibiotics also can predispose individuals to this condition. Further, those with excessive pronation or flat arches face an elevated risk due to the heightened demands placed on the tendon during regular walking. Whether involved in regular labor-intensive work or sporadic intense physical activities, individuals must be mindful of the strain placed on their Achilles tendon. If you have pain in the back of the heel, it is suggested that you make an appointment with a podiatrist.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact Dr. Janet Leicht of New Jersey. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
Rupture Symptoms
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
If you have any questions please feel free to contact our office located in Berkeley Heights, NJ . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.